We Care Because You Care
Dove Creek Animal Hospital in Denton, Texas offers a myriad of veterinary services for your pets.
Cat Services
Kitten Care
Cat Senior Care
Cat Adult Care
Cat Dental Care
Cat Flea & Tick
- Cat Heartworms
Cat Preventative Care
Cat Spay
Cat Neuter
Cat Vaccinations
Cat Microchip
Cat Bath
Cat Orthopedic Surgery
Dog Services
Puppy Care
Dog Senior Care
Dog Adult Care
Dog Dental Care
Dog Flea & Tick
Dog Heartworm
Dog Microchipping
Dog Vaccinations
Dog Spaying
Dog Neutering
Dog Bath
Dog Orthopedic Surgery

Our Treatments
Our office offers early detection testing for many illnesses and conditions. Contact us for more details.
Dove Creek Animal Hospital has partnered with Dr. Kaitlyn Lackey, a certified Veterinary chiropractor (https://www.instridechiropractic.com/). Adding in chiropractic adjustments to many of our patient’s treatment plans has resulted in more comfort, less pain and an overall better quality of life. In order to begin chiropractic treatment your pet must be evaluated by a veterinarian and must have a signed referral form. Some ailments may not benefit from chiropractic adjusting which is why an evaluation by a licensed veterinarian is required at this time. Please call to schedule an appointment today for possible chiropractic referral.
We offer a large variety of Nutritional Counseling for pets of all stages. This will include weight consults, discuss of proper diet for your pets needs. Listed below are the diets we carry in our Hospital, but not limited to additional brands.
Hill’s Science Diet Prescription Foods and Treats for Canine & Feline
Hill’s Science Diet Non-Prescription Foods and Treats for Canine & Feline
Royal Canin Prescription Foods for Canine & Feline
Come to the front of the line! We will always address emergencies with top priority and after hours we refer our clients to the Denton County Animal ER.
Laboratory Work
Click Here To Read More About Our Laboratory, Radiology, & Ultrasound Work
In House Lab Work
- CBC
- Chemistry
- Heartworm Testing
- FIV/FeLV Testing
Radiology
- Digital
Cytology
- Intestinal Parasite
- Otitis Testing (Ears)
- Skin (Mites)
Laboratory, Radiology, & Ultrasound
Imaging Tests (Radiology Options) for Pets
Date Published: 08/13/2010
Date Reviewed/Revised: 01/11/2019
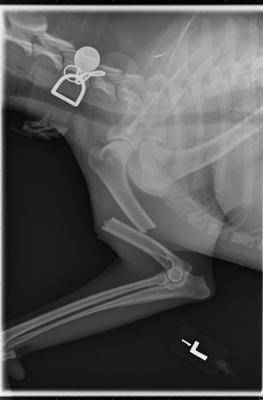
Radiograph, or x-ray, of a broken humerus. Photo by Dr. John Daugherty
Imaging in veterinary medicine has advanced greatly since the first radiographs (x-rays) were taken of pets just decades ago. Today a multitude of imaging tests are available to help diagnose and treat diseases in our pets. These tests include radiography (x-rays), ultrasound, CT (or CAT) scans, and MRI scans. Each of these tests has its own advantages and disadvantages, and will provide the veterinarian with different information. Many of these tests are available in general veterinary practices, but some, such as CT and MRI scans, are most often performed by specialists in large referral practices or veterinary schools.
As with all tests, none of them is perfect for every situation. The following is a brief description of different types of imaging.
Radiograph/X-ray
A radiograph, commonly called an x-ray, is a black and white two-dimensional image of part of the interior of a body. An image is generated by passing radiation through a particular structure or area, such as the chest or a limb, and the image is then captured. The traditional way of recording the image is on specific x-ray film that senses how much radiation passes through the structure and reaches the film, much like photographic film captures light. The denser a tissue is (such as bone), the whiter the image is on the film. Less dense structures, such as air in the lungs, allow almost all of the x-ray energy to pass through to the film, turning that area black.
In the past 10-12 years, many practices have upgraded to digital radiography. The principles are similar, but the images are captured on a digital recording device and displayed on a computer screen. No x-ray film is used. These images are easy to store as well as to transmit to other hospitals, or to copy to send home with pet owners. Not much more than a decade ago, these systems were considered to be too expensive for most private veterinary hospitals, but they are now being used in the majority of practices. As with most technology, the cost of installing a digital system has fallen as demand for them has increased.
Regardless of whether the images are on film or digital, radiography is the most common and readily available imaging test in veterinary practice. It is used to evaluate the size and shape of organs, such as the heart and lungs, as well as to demonstrate broken bones, some foreign objects, fluid accumulations, and many more abnormalities that may aid in diagnosis. It is also the most affordable imaging test, and is most often done prior to any of the other imaging options.
Contrast Studies
There is a subcategory of x-ray studies that use contrast dyes that show up on radiographs to highlight certain structures. The most familiar of these is the barium series, in which either a liquid or a paste containing barium is given orally or by enema to a patient to highlight a part of the gastrointestinal (GI) tract. Because some objects do not show up on radiographs (such as plastic, cloth, toys, rubber, etc.), barium can help diagnose obstructions or blockages. Barium shows as bright white on radiographs, so if it reaches a certain point in the GI tract and stops abruptly, we can infer that there is something blocking its progress. Sometimes we can also see a foreign object outlined by the barium trying to get around it.
The reason it is called a barium “series” is because it’s necessary to take a series of x-rays at timed intervals as the barium goes through the stomach and intestines to the large intestines. The amount of time the series must be continued depends on what is found, but it can take up to 24 hours to complete in some cases, so usually the pet is hospitalized for the day. Some patients may even need to return to the hospital the next day for follow-up.
A barium study can be done in any clinic that has radiographic equipment and liquid barium. However, if the pet is vomiting so much that the barium cannot be retained in the GI tract, the test may not be useful.
Another example of a contrast study is the intravenous pyelogram (IVP) in which a dye is injected intravenously. This dye is filtered from the blood by the kidneys and excreted through the urinary tract, so a series of images is taken to show its progress through the kidneys and into the ureters and bladder. This progress can be helpful to demonstrate structural kidney diseases, ureters that are abnormally large or don’t enter the bladder in the correct place, and for certain bladder diseases.
There are other contrast studies that can be done, including cystograms, a dye placed in the bladder through the urethra by catheterization; myelography, a dye around the spinal cord; and more.
Ultrasound (Sonogram)
Unlike radiographs, no radiation is used in an ultrasound study. An ultrasound machine uses sound waves. The ultrasound waves move out from the wand and either become absorbed into organs, pass through them, or are reflected (echo) back. Depending on how many sound waves are absorbed or reflected, an image of the internal organs is formed by a sophisticated integrated computer, and the image is then displayed on a monitor. Real-time moving images are displayed, and still images can be captured as well.
Ultrasound is painless and does not require anesthesia or even sedation in most cases. For an ultrasound evaluation to be done, the pet does need to have the hair shaved from the evaluation area because it will interfere with the images.
This test is typically done after blood tests, x-rays, or a physical examination indicates a possible problem. It is useful for evaluating abdominal organs, eyes, and the reproductive system. As with people, it can be used during pregnancies. A specific ultrasound called an echocardiogram is used to visualize the heart and blood vessels as well as its valves.
Ultrasound can “see” some things that can’t be visualized on radiographs. For example, if the abdomen is filled with fluid, the organs can’t be distinguished on traditional x-rays because fluid and tissue have the same density. However, they appear quite different from each other on an ultrasound image, so we can see through the fluid. It is also useful, for the same reason, for seeing inside an organ such as the heart or liver.
On the other hand, it is not as good at seeing through air or bone, so it does not replace radiography but rather is complementary to the information we can get from radiographs. It is common to do both x-rays and ultrasound in order to get a good picture of what is going on.
Because the equipment can be expensive, not all veterinary hospitals have an ultrasound machine. However, in those cases, they can often arrange for a traveling ultrasonographer to come to the hospital. If this is not an option, then the pet can be referred to a hospital that has one. Ultrasound images are different than x-ray images, and in some cases, it may be preferable for a veterinarian who is experienced in obtaining and reading ultrasound images to do the evaluation, or in some cases, to have a board-certified veterinary radiologist do the procedure.
As with radiography, there is also a subset of ultrasound imaging tests called contrast ultrasonography in which a material that is visible to ultrasound waves is injected as the image is being watched on the screen. These procedures are usually performed by a specialist.
General Services
Early Detection Testing
Nutritional Counseling
Pet Emergency

Vaccinations

Regular Check Ups

Emergency Care
If you have any other questions, please contact us
“I recently moved from Kansas and was searching for a new Vet. The staff were friendly and got us in quickly. Front desk staff were courteous and efficient. Veterinarian was super nice and explained everything very well. Felt more comfortable at Dove Creek and more like home.”

“Best Veterinary hospital I have taken my pets too in a long time. Dove Creek has the best and most caring staff. The Doctor’s and staff are very knowledgeable and considerate of your situation. I highly recommend Dove Creek Animal Hospital.”

“I actually went to the wrong location and am so glad i did! Our Vet Tech and Dr. Hill were very caring and thorough. I will definitely return and I know EXACTLY where Dove Creek is located now. Thank you for all the attention and care you showed to me and my sweet old Golden”

Professional Pet Care
Pet owners trust us to look after the needs of their beloved companions. We are specialists committed to delivering the very highest of veterinary care and affection.

